eye Insights Issue 04: Genetic Testing
 In eye Insights™ Issue 4, Massachusetts Eye and Ear specialists publish vital information about the usefulness of genetic diagnostic testing for eye diseases. Janey Wiggs, MD, PhD, provides guidelines for integrating genetic diagnostic testing into clinical care for patients with inherited retinal degenerations, early-stage glaucoma, and primary optic atrophy. Also includes information on how to order tests through the Ocular Genomics Institute at Mass. Eye and Ear. Created to educate and inform ophthalmologists about various topics in ophthalmic care, Eye Insights is sponsored by Mass. Eye and Ear and Massachusetts General Hospital, and mailed to more than 18,500 practicing ophthalmologists across the nation.
In eye Insights™ Issue 4, Massachusetts Eye and Ear specialists publish vital information about the usefulness of genetic diagnostic testing for eye diseases. Janey Wiggs, MD, PhD, provides guidelines for integrating genetic diagnostic testing into clinical care for patients with inherited retinal degenerations, early-stage glaucoma, and primary optic atrophy. Also includes information on how to order tests through the Ocular Genomics Institute at Mass. Eye and Ear. Created to educate and inform ophthalmologists about various topics in ophthalmic care, Eye Insights is sponsored by Mass. Eye and Ear and Massachusetts General Hospital, and mailed to more than 18,500 practicing ophthalmologists across the nation.
Inside:
Sensitive and specific genetic tests now exist for dozens of inherited eye diseases. So, what tests are available, and when are they appropriate for your patients?
- Welcome letter
- Frequently asked questions about genetic testing
- When is genetic testing appropriate?
- General guidelines for genetic testing
- Genetic testing services at Mass. Eye and Ear
- Integrating genetic testing into clinical care
- Meet the experts and related reading
Editor-in-Chief: Joan W. Miller, MD
Managing Editor: Matthew F. Gardiner, MD
Clinical Advisory Group: Carolyn E. Kloek, MD, Deeba Husain, MD, Ankoor S. Shah, MD, PhD, Angela V. Turalba, M
Communications Director: Suzanne Ward
Scientific Communications Manager: Wendy Chao, PhD
Publications Manager: Wendy Weissner
Graphic Design: Beth Durkee
Contributors: Janey Wiggs, MD, PhD, and Emily Place, MS, LCGC
| eye Insights 4 PDF | 4.43 MB |
Welcome Letter
Dear Colleagues:
The accelerated pace of molecular discoveries during the past two decades, coupled with an evolving “precision medicine” model in healthcare, are fueling an increase in the number of people who undergo genetic testing. In Ophthalmology, genetic testing is still in its early stages, but already is transforming our ability to pinpoint the cause of some inherited eye diseases that result from single gene mutations, such as retinitis pigmentosa. In many cases, genetic testing can help your patients and their families better understand their risk for disease, likelihood of disease progression, and options for treatment. It can also help them make more informed decisions about their health.
Sensitive and specific genetic tests now exist for dozens of inherited eye diseases. In this issue of Eye Insights we explore what tests are available, and provide guidelines for assessing when genetic testing may benefit your patients and how it can be incorporated into your clinical care practice.
The Harvard Ophthalmology Ocular Genomics Institute (OGI), based at Massachusetts Eye and Ear, offers comprehensive genetic diagnostic testing for inherited eye diseases, including inherited retinal degenerations, early-onset glaucoma, and primary optic atrophy, via several Genetic Eye Disease (GEDi) tests. As described in a paper published in the journal Genetics in Medicine, analyses performed by the OGI team show that GEDi testing provides more accurate diagnoses than other testing methods; this can improve genetic counseling and facilitate the use of focal ocular treatments and therapies, including gene therapies. Our service is CLIA-certified, and we invite you to learn more.

Joan W. Miller, MD, FARVO
Henry Willard Williams Professor of Ophthalmology
Chair, Harvard Medical School Department of Ophthalmology
Chief of Ophthalmology, Massachusetts Eye and Ear and
Massachusetts General Hospital
Genetic Testing FAQs
What are the benefits of genetic testing?
Genetic tests can help to:
- Diagnose disease
- Improve the accuracy of a patient’s prognosis and genetic counseling
- Identify gene mutations that could be passed on to children
- Screen newborn babies for certain treatable conditions
- Identify mutations presymptomatically. For some diseases, including early-onset glaucoma, this allows for increased disease surveillance and timely treatment.
What is required for a genetic test?
Genetic testing requires a tissue sample from the patient, usually blood or saliva, which is sent to a CLIA-certified laboratory for testing.
What factors should I consider before ordering a test?
- Usefulness: Consider whether or not testing will help you better manage your patient, including the opportunity for gene-based therapies as they become more readily available. Genetic testing is particularly useful for patients who have a family history of inherited retinal degenerations, early-onset glaucoma, and primary optic atrophy.
- Cost: For many patients, affordability is an important consideration and should be factored in to the decision-making process. Costs versus benefits also should be considered. In some cases, an expedited test result (a more expensive option) may allow more rapid access to effective therapy or to information that is needed for family planning. At Mass. Eye and Ear, costs range from $500 to $3,500 depending on the type of test. Health insurance may cover part or all of the costs.
- Turnaround Time: This varies laboratory to laboratory, and will depend upon the type of test ordered. Typical turnaround time at Mass. Eye and Ear is 90 days.
- Reporting: Patients should receive written copies of each genetic test report. Reports are returned to the physician who ordered the test and should be interpreted by a health care provider with knowledge of the disease genetics.
When is Genetic Testing Appropriate?
Many inherited diseases are caused by mutations in a single gene (Mendelian disorder), and detection of the responsible mutation can predict development of the disease with relatively high accuracy. If your clinical findings suggest the presence of an inherited eye disease, such as those described below, genetic testing is worth considering and discussing with your patient.
Some heritable disorders are complex, meaning that they are the result of multiple genetic and environmental factors. The presence of any one of the disease-associated gene variants in complex disorders, such as age-related macular degeneration, may not be highly predictive of the development of the disease. In these cases, standard diagnostic methods such as biomicroscopy, ophthalmoscopy, tonography, and perimetry – rather than genetic testing – will more accurately assess a patient’s risk of vision loss.
Inherited Retinal Degenerations
Patients with clinical features of inherited retinal degenerations can benefit from genetic testing. Identifying disease-causing mutations aids genetic counseling by establishing the inheritance pattern (autosomal dominant, recessive, X-linked, or mitochondrial [maternal] inheritance), and identifying patients who are eligible to take part in clinical trials evaluating gene-based and cellular therapies. Many patients with inherited retinal degenerations have similar clinical features. For this reason, the GEDi-R panel is the most efficient method of screening, simultaneously testing 250 genes known to cause retinal degenerations.
Early-onset Glaucoma
When glaucoma develops in a patient before age forty (early-onset glaucoma), the disease is more likely to be caused by one of eight known high-risk genes. Early-onset glaucoma genes contribute to a broad range of phenotypes that can be difficult to distinguish by clinical features alone. The most efficient method to screen for early-onset glaucoma gene mutations is to use a panel test, such as GEDi-O, that simultaneously screens all eight genes. This information can aid genetic counseling by defining the inheritance pattern and identifying mutation carriers presymtomatically.
Primary Optic Atrophy
Approximately 50 percent of patients with primary optic atrophy have disease-causing mutations in either the OPA1 gene (inherited as a dominant trait and causing Kjer optic neuropathy), or mitochondrial DNA (inherited through maternal lineage and causing Leber Hereditary Optic Neuropathy). Nine other gene variants with dominant or recessive inheritance traits are also known to cause optic atrophy. Therefore, identifying the patient’s disease-causing genes will help define the inheritance pattern and phenotype. Since primary optic atrophy can overlap phenotypically with the normal tension type of glaucoma, it is useful to screen patients for both optic atrophy and glaucoma genes using the GEDi-O panel test. Additionally, clinical trials of gene therapy for specific genetic forms of optic neuropathy are in progress; genetic testing can help determine if patients are eligible for these studies.
For further reading, please see: Wiggs JL, Pierce EA. Genetic testing for inherited eye disease: who benefits? JAMA Ophthalmol. 2013 Oct;131(10):1265-6.
General Guidelines for Genetic Testing
- Offer genetic testing to patients whose clinical findings suggest a Mendelian disorder with a known gene mutation.
- If you are unfamiliar with the specific testing required, encourage the involvement of a board-certified medical geneticist, genetic counselor, or both for all genetic tests. This will help to ensure accuracy of testing and interpretation of results, and that proper counseling is provided to the patient.
- Use Clinical Laboratories Improvement Amendments (CLIA)–approved laboratories for all clinical testing to ensure accuracy and quality of testing.
- Provide a copy of each genetic test report to the patient. This information allows patients to independently search for mechanism-specific information, such as the availability of gene-specific clinical trials.
- Consider panel testing for disorders that can be caused by mutations in more than one gene.
- Avoid direct-to-consumer genetic testing and discourage patients from obtaining such tests themselves.
- Avoid routine genetic testing for genetically complex disorders like age-related macular degeneration and late-onset glaucoma.
- Avoid testing asymptomatic minors for untreatable disorders except when surveillance or lifestyle modifications can be beneficial.
Genetic Testing Services at Mass. Eye and Ear
Genetic testing can be ordered only by a medical professional. Blood is the preferred specimen for testing. CLIA-certified genetic testing services provided by the Ocular Genomics Institute at Mass. Eye and Ear range from $500-$3,500. Health insurance may cover part or all of the cost. A typical turnaround time is 90 days.
- Genetic Eye Disease panel for Retina genes (GEDi-R) - Inherited retinal degenerations and related disorders
- Genetic Eye Disease panel for Optic nerve genes and early onset glaucoma (GEDi-O)
- Genetic Eye Disease panel for Strabismus genes (GEDi-S)
- Confirmation of research finding or familial variant testing
For inquiries and test requisition forms, visit us here.
Integrating Genetic Testing into Clinical Care
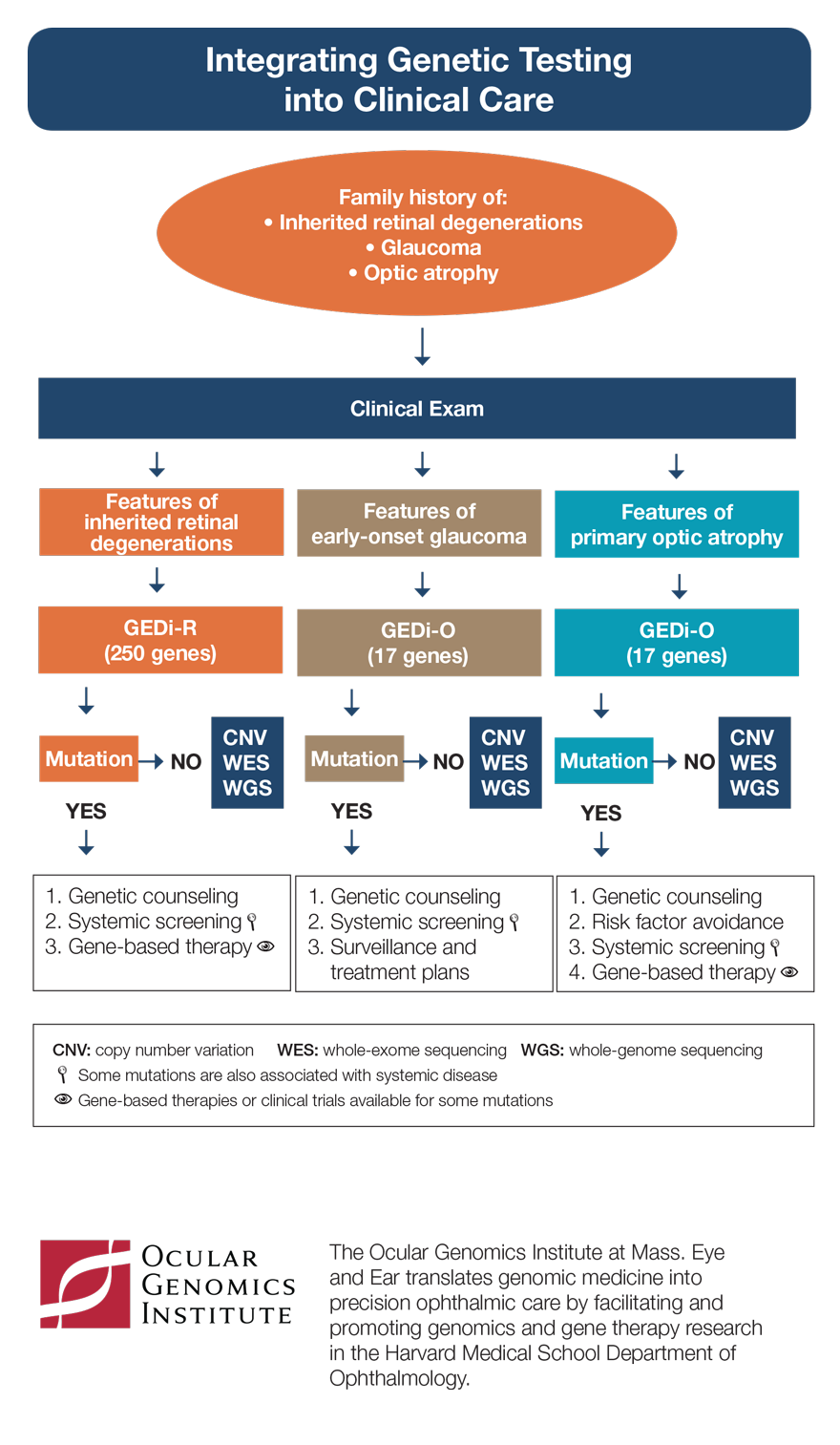
Meet the Experts and Related Reading
Meet the Experts

Janey Wiggs, MD, PhD
Associate Director of the Ocular Genomics Institute at Mass. Eye and Ear
Paul Austin Chandler Professor of Ophthalmology at Harvard Medical School
Dr. Wiggs is a board-certified medical geneticist specializing in the genetics of glaucoma with particular interest in complex and advanced glaucoma, and inherited ocular disorders. She directs the CLIA-certified clinical diagnostic genetic laboratory at Mass. Eye and Ear, where patients are tested for mutations in genes that can cause inherited retinal disorders, early-onset glaucoma, or primary optic neuropathy.
 Eric Pierce, MD, PhD
Eric Pierce, MD, PhD
Director of the Ocular Genomics Institute at Mass. Eye and Ear
Sol and Libe Friedman Associate Professor of Ophthalmology at Harvard Medical School
Dr. Pierce seeks to improve our understanding of the molecular bases of inherited retinal degenerations so that rational therapies can be developed for these diseases. As a clinician scientist, he conducts clinical research and laboratory-based investigations of retinal biology and disease, and provides clinical care for children and adults with retinal degenerative disorders. He is currently working to develop gene therapy for several forms of inherited retinal degenerations.
Related Reading
- Stone EM, Aldave AJ, Drack AV, Maccumber MW, Sheffield VC, Traboulsi E, Weleber RG. Recommendations for genetic testing of inherited eye diseases: report of the American Academy of Ophthalmology task force on genetic testing. Ophthalmology. 2012 Nov;119(11):2408-10.
- Wiggs JL, Pierce EA. Genetic testing for inherited eye disease: who benefits? JAMA Ophthalmol. 2013 Oct;131(10):1265-6.
