Advances in postoperative care have greatly improved the clinical success of the Boston KPro. Common complications such as inflammation and infection are significantly lower with today’s prophylactic drug regimens. Innovative devices have also improved postoperative management of KPro. Soft contact lenses are now worn continuously to enhance graft retention, and prevent irritation and evaporative damage.
Prophylactic Antibiotic Regimen
Daily antibiotics are recommended for life and regimens are subject to regional availability, cost and bacterial resistance. Option 1 is preferred at Mass. Eye and Ear. Polytrim™ is presently less expensive than 4th-generation fluoroquinolones. If antibiotics are unavailable, 1% povidone iodine 2 to 4 times daily can be used for the short-term. Patients should be cautioned to avoid eye rubbing, as infectious or toxic debris may be pushed into the eye.
Non-Autoimmune Patients:
- Option 1 - Polymyxin B / Trimethoprim (Polytrim™) 1 x /day
- Option 2 - Fluoroquinolone (4th generation) 1 x /day
- Option 3 - Fluoroquinolone (4th generation) and Vancomycin 1 x /day
Autoimmune or Monocular Patients:
- Option 1 - Polymyxin B / Trimethoprim (Polytrim™) and Vancomycin 1-2 x /day
- Option 2 - Fluoroquinolone (4th generation) and Vancomycin 1 x /day
- Option 3 - Fluoroquinolone (4th generation) and Chloramphenicol 1 x /day
Fungal Prophylaxis
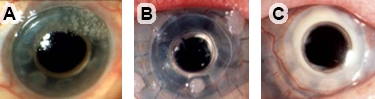
Signs of fungal presence include mulberry shaped deposits on soft contact lens (colonization, figures A and B) and a white sheen around the stem (keratitis infection, figure C). If fungal infection is suspected, discontinue steroids before treating with anti-fungals. Additionally, the contact lens should be replaced if any signs of fungal colonization or infection occur.
- Option 1 - Amphotericin B (0.15%) 2 x / day for 1 week (every 3 months)
- Option 2 - Natamycin (5%)
Corticosteroids
To control inflammation after KPro implantation, prednisolone 1% drops 2-4x per day for the first month are recommended. After the first month, taper to adjust for level of inflammation.
Soft Contact Lenses
After KPro implantation, a large, soft contact lens worn as extended wear is preferable. Contact lenses will need to be worn constantly for life. Lenses can be any Dk and any diameter and curve that fits.
Troubleshooting Common Contact Lens Problems
- If retention is a problem, increase diameter of soft contact lens to 18-22mm or refit with hybrid lens.
- If soft contact lens is clear (no deposits), routine replacement is not necessary. Mass. Eye and Ear recommends cleaning every 3-6 months in the clinic.
- If repeated vision-impairing deposits build up, requiring frequent replacement of the soft contact lens, switch to a hybrid lens (rigid gas permeable center with soft periphery).
- If conjunctival erosion develops over the tube of a glaucoma shunt and not the plate, increase the diameter of the soft contact lens and add Vancomycin drops if on Polytrim™ alone.
- If there is significant mucus associated with the erosion, or if the erosion does not heal in 1-2 months after the soft contact lens change, consider surgical repair.
Glaucoma and Boston KPro
Ideally managed jointly with a glaucoma specialist, the prevention of glaucoma after Boston KPro surgery should be considered a priority at the time of KPro evaluation and during each postoperative visit.
- Prior to KPro Surgery: Consider treating patients with glaucoma with eye drops prophylactically. If glaucoma is diagnosed prior to KPro surgery, consider Ahmed™ valve shunt implantation before, or simultaneously with, KPro implantation. Mass. Eye and Ear recommends creating a long scleral tunnel and placing the tube into the anterior chamber. The tube can also be placed in the pars plana if the patient had a full vitrectomy.
- After KPro Surgery: Target low intraocular pressure—ideally 7 - 15 mmHg by finger palpation, depending on glaucoma stage. Consider performing Ahmed™ valve shunt implantation early if intraocular pressure rises or if the cup to disc ratio increases.
-
Frequency of Tests:
- Intraocular Pressure - Repeat every 3 months
- Cup to Disc Ratio - Repeat every 3 months
- Visual Field - Repeat every 3 months
- Retinal Nerve Fiber Layer Measurement - Repeat every 6 months
- Disc Photos - Repeat every 12 months
